© Author: Z. Nelly Vladimirovna, doctor at the Research Institute of Transfusiology and Medical Biotechnology, especially for SosudInfo.ru (about the authors)
Vasodilators or vasodilators are a group of medications produced in various dosage forms (tablets, capsules, injection solutions), belonging to various pharmaceutical groups and prescribed for arterial hypertension and many pathological conditions of the vessels of the brain, heart, spine, upper and lower limbs.
Diverse group
Vasodilator drugs are capable of influencing vascular walls in various ways (depending on their mechanism of action), reducing their tone and, due to this, increasing the diameter of blood vessels, improving blood flow in them. However, not all pharmaceuticals classified in this category affect different types of blood vessels to the same extent. The “competence” of each of the groups of these medications includes vessels of a certain caliber (arterioles, arteries, venules, great vessels) and belonging to specific tissues and organs.
dilation of the vessel and improvement of blood flow under the influence of a vasodilator
For example, to dilate small vessels of the microvasculature of organs such as eyes, kidneys, some drugs are used, and to influence small vessels of the skin, upper and lower extremities, other vasodilators (peripheral vasodilators) are used.
In this case, it can be assumed that the heart vessels are unlikely to “feel” the effect of previous drugs; they need their own, special drugs, which is actually what happens. To dilate the coronary vessels in the treatment of angina or heart failure, drugs from the group of cardiac vasodilators are prescribed. In general, taking into account the mechanism of action and the vessel (arterial or venous bed), which is predominantly influenced by vasodilators, three subgroups of vasodilator drugs are distinguished:
- Drugs acting on arterioles (direct arterial vasodilators): alpha-non-selective adrenergic blockers (AB), hydralazine, calcium antagonists;
- Medicines whose “circle of interest” includes venules: organic nitrates (nitroglycerin, nitrong);
- Drugs that have a simultaneous effect on some (arterioles) and other (venules) vessels: inorganic nitrates, alpha-1-nonselective ABs.
In addition, the modern pharmacological industry also has vasodilators that are endowed with the ability to increase the lumen of large-caliber vessels and highways. These are systemic vasodilators; they are able to quickly reduce blood pressure and increase the intensity of blood supply in all tissues of the body.
applicability of vasodilators depending on the pharmacological group
Before prescribing drugs of one group or another, the doctor studies not only the patient’s condition caused by the pathological process occurring in his body, but also takes into account the condition of the patient’s blood vessels.
No. 12. Direct vasodilators in the treatment of arterial hypertension
You are reading a series of articles about antihypertensive (antihypertensive) drugs. If you want to get a more holistic view of the topic, please start at the beginning: an overview of antihypertensive drugs that act on the nervous system.
When talking about drugs used in the treatment of hypertension (arterial hypertension), one cannot miss the group of direct vasodilators
, because without it the review will not be complete enough.
Vasodilator
(emphasis on the penultimate syllable) in literal translation means “
expanding vessel
”, “
vasodilator
” (from Latin
vas
,
vasis
- vessel,
dilatatio
- expansion).
According to the rules of the Latin language, the Latin letter l
denotes a soft sound [
l
], therefore it is more correct to use the term
vasodil
I tators
, but the Latin language is studied in the 1st year and is largely forgotten by the end of medical school. I will use the more common version with a hard [ l
].
Vasodilators by mechanism of action
divided into direct and indirect.
Indirect vasodilators
include:
- alpha1-blockers and non-selective alpha-blockers,
- serotonin receptor blockers,
- calcium antagonists,
- ACE inhibitors
(an important group of drugs, we will talk about it later), etc.
To direct vasodilators
, which directly dilate blood vessels include 4 typical drugs (
hydralazine, minoxidil, diazoxide, sodium nitroprusside
) and a group
of nitrates
(
nitroglycerin,
etc.). Nitrates are a separate important group of drugs used to relieve ischemic pain in angina pectoris; a separate discussion is needed about it.
Thus, currently under direct vasodilators
Usually they mean only
4 drugs
:
- hydralazine,
- minoxidil,
- diazoxide,
- sodium nitroprusside.
What you want to know
from today's topic?
- The first three drugs ( hydralazine, minoxidil, diazoxide
) dilate
only small arteries
(arterioles), while sodium nitroprusside also dilates
venous vessels
. - All 4 drugs have a large number of side effects
(some of them are very interesting!) and are rarely used for the treatment of arterial hypertension. - All direct vasodilators cause fluid retention
in the body (edema) and
palpitations
(tachycardia). - Hydralazine
(more precisely, an analogue
of dihydralazine
) is part of the combination drugs:
adelfan
and
adelfan-esidrex
. It is not advisable to use them for a long time. - The use of minoxidil
internally has revealed an unusual side effect - increased hair growth, so minoxidil is now used externally to treat
male pattern baldness
(androgenetic alopecia). - Diazoxide
also has a rare side effect: it
inhibits the secretion of insulin
by the pancreas and is therefore used in endocrinology to increase blood sugar levels. - Sodium nitroprusside
is administered only intravenously, it acts quickly, but for a very short time.
Since sodium nitroprusside breaks down into cyanide, an overdose of it is very similar in appearance to a coma caused by carbon monoxide
(CO) poisoning.
And now for each drug in a little more detail.
Hydralazine
Hydralazine is a direct peripheral vasodilator acting on arterioles. Vasodilation is associated with inhibition of phosphorylation of myosin, a protein involved in muscle contraction. Hydralazine causes reflex tachycardia
(increase in heart rate).
With prolonged use, tolerance
(addiction) to the action of hydralazine develops.
Research in the USSR in 1985-1988. showed that monotherapy with hydralazine for 1 year was ineffective
y with mild and moderate hypertension (the effect was achieved in only 23% of patients compared to 50% with propranolol).
With significant hypertension (lower blood pressure above 114 mm Hg), hydralazine did not help in any case
.
Hydralazine is not available in pharmacies and is not used
due to low effectiveness and many side effects.
It can be prescribed as an additional drug in combination with diuretics
and beta-blockers. In older people it should be used in a lower dosage.
Hydralazine currently retains some importance because pharmacies still sell inexpensive combination antihypertensive drugs in tablet form: adelfan
and
adelfan-esidrex
(I wrote more about them in the topic about sympatholytics).
About 20 years ago, adelfan
was very popular among pensioners, because there were few other more or less effective drugs for hypertension.
In addition to dihydralazine
,
adelfan
contains the sympatholytic
reserpine
, while
adelfan-esidrex
additionally includes the common diuretic
hydrochlorothiazide
.
Dihydralazine differs from hydralazine in its greater predictability of effect
, since the rate of breakdown of dihydralazine in the body does not depend on the genetic characteristics of the patient (there are so-called
fast
and
slow acetylators
).
Side effects
hydralazine:
- due to reflex sympathetic stimulation of the heart and kidneys, tachycardia
and
edema
(fluid retention in the body) occur, - ischemic changes on the ECG are possible up to the development of myocardial infarction (this is reminiscent of the side effects of nifedipine),
- after 0.5-2 years of treatment, autoimmune reactions
. In 80% of cases, these are arthritis (inflammation of the joints) and arthralgia (pain in the joints), but there are also glomerulonephritis (inflammation of the renal glomeruli), lupus syndrome (reminiscent of systemic lupus erythematosus), etc. - thrombocytopenia
(a decrease in the number of platelets in the blood) and even
pancytopenia
(a decrease in the number of all cells in the blood) are possible - peripheral neuritis, neuropathy
(nerve damage).
In this case pyridoxine
(vitamin B6) should be prescribed. - gastrointestinal disorders (nausea, diarrhea),
- skin rash,
- impotence,
- lacrimation or conjunctivitis,
- nasal congestion, etc.
The abundance of side effects, including autoimmune ones, does not allow the use of the combined drug Adelfan
(adelfan-esidrex) long-term.
Minoxidil
Minoxidil, like hydralazine
, has a direct vasodilator effect on the arteries.
Since the drug does not dilate the venous bed, it does not cause orthostatic hypotension
(
a sharp drop in blood pressure with fainting when moving from a horizontal to a vertical position
).
A decrease in blood pressure is accompanied by reflex tachycardia
and an increase in
stroke volume
(
the amount of blood in ml ejected by the heart per contraction
), as well as
sodium and water retention
(edema). Minoxidil has a renoprotective effect (protects the kidneys from the effects of high blood pressure).
Due to the numerous side effects of minoxidil
(tablets)
is not currently used for the treatment of arterial hypertension
, despite its effectiveness even in hypertensive crises.
The effect of the drug does not occur quickly enough (onset after 0.5-1 hour, peak after 4-8 hours). Minoxidil is considered a 4th line treatment for hypertension and is usually prescribed only in combination with beta blockers
or
ACE inhibitors and diuretics
.
Side effects
minoxidil when used orally and parenterally (i.v., i.m.):
- tachycardia and palpitations (due to reflex stimulation of the sympathetic nervous system),
- swelling and fluid retention,
- decrease in the ST segment and changes in the T wave in leads I and V4-V6 (in 90% of cases in the first 2 weeks),
- angina pectoris, myocardial infarction,
- effusion pericarditis ( inflammation of the pericardium with accumulation of fluid in the cavity of the pericardial sac
) due to fluid retention and inadequate increase in blood flow in the pericardium and myocardium, - pulmonary hypertension,
- throbbing headache, blurred vision,
- temporary increase in blood levels of alkaline phosphatase, urea, creatinine,
- gastrointestinal disorders,
- polymenorrhea ( heavy periods
), - skin rash, etc.
gynecomastia may also occur.
(
enlargement and thickening of the mammary gland buds in men, often painful
), sexual dysfunction.
Particular attention should be paid to such a side effect as hypertrichosis
(
excessive hairiness
) and
hirsutism
(
excessive growth of dark, coarse, long male-pattern hair in women
).
Hypertrichosis occurs in almost all patients when taking minoxidil orally for more than 4 weeks - hair grows on the temples, forehead, face, ears and other hairy areas of the body. This is due to increased levels of testosterone
(male sex hormone) and increased skin blood flow. Hypertrichosis and hirsutism limit the use of the drug in women, although this goes away within 1-2 months after stopping use.
Minoxidil's ability to induce hair growth is now used specifically to treat androgen-dependent alopecia.
(male pattern baldness).
When applied topically ( Rogaine
,
Generalolon
, etc.), minoxidil is almost not absorbed and therefore does not have the usual side effects. It is believed that hair growth is associated with vasodilation and improved blood circulation and nutrition of hair follicles in the skin, which stimulates their transition from the resting phase to the growth phase.Maximum effect
minoxidil is achieved at the beginning of baldness (no later than 10 years, preferably before 3-5 years), in young patients, when the bald spot is localized in the crown area no more than 10 cm in size and there are more than 100 hairs of different types in the center of the bald spot. Minoxidil is ineffective for hair loss due to medications, nutritional disorders (deficiency of vitamin A, iron, etc.), tight hairstyles (“ponytail”, “bun”). Hair growth usually begins after 4 months of daily treatment. After discontinuation of the drug, new hair growth stops and after 3–4 months the bald patches can be restored to their original places.
Diazoxide
Diazoxide's chemical structure is a derivative of thiazide diuretics
(this includes
hydrochlorothiazide
), although it itself does not have a diuretic effect.
Like other direct vasodilators, it causes sodium and water retention
(edema is possible). Acts only on arterioles. When administered intravenously, diazoxide quickly reduces systolic and diastolic blood pressure with an increase in heart rate and therefore can be used to treat hypertensive crises when other drugs are ineffective.
Diazoxide inhibits insulin secretion
from the pancreas, which leads to an increase in blood sugar levels, so the drug is now used mainly for
the treatment of congenital hyperinsulinism
(occurs in 1 in 50 thousand people).
Diazoxide also has a strong relaxing effect on the uterus.
. If the drug is administered during labor, labor will stop.
Side effects
diazoxide:
- swelling and heart failure (more often in children),
- hypotension, tachycardia, myocardial ischemia,
- skin rash,
- ketoacidosis,
- changes in taste sensations, nausea and vomiting,
- hypertrichosis, hirsutism,
- headache, dizziness, tinnitus,
- changes in blood cell content, etc.
Sodium nitroprusside
Direct dilator of arterioles and veins
(unlike the three previous ones, which act only on arterioles).
Sodium nitroprusside is used only intravenously
and has an immediate (30-60 seconds) effect, although it is short-lived and
ends within 3-5 minutes
after stopping the infusion. The drug increases heart rate to a small extent.
Sodium nitroprusside reduces the load on the heart well and is therefore especially effective in acute left ventricular failure.
caused by high blood pressure.
The drug dilates the blood vessels of the heart and improves blood supply to the myocardium during heart attack and unstable angina. The hypotensive effect of sodium nitroprusside is due to the nitroso group, so the effect of the drug is similar to the effects of nitroglycerin
. Sodium nitroprusside inhibits platelet aggregation, i.e. slows down blood clotting and blood clot formation.
Flaws
sodium nitroprusside:
- high price,
- the need for precise dosing (special dispensers
) with careful monitoring of blood pressure, - after stopping the infusion, a severe withdrawal syndrome
with a rise in blood pressure is possible, - side effects.
Dispenser-infusion pump
. The motor of the device presses on the syringe piston at an adjustable speed; the drug solution is constantly fed through a tube into the dropper and administered intravenously to the patient.
Indications
for the use of sodium nitroprusside:
- hypertensive crises,
- controlled hypotension during surgery,
- acute myocardial infarction without hypotension,
- arterial spasms resistant to nitroglycerin.
Sodium nitroprusside is converted into cyanide
, they, in turn, react with thiosulfates in the blood and are converted into
thiocyanates
, which are then excreted by the kidneys within a few days.
Cyanides are toxic
because
are salts of a powerful poison - hydrocyanic acid
, which blocks the enzyme
cytochrome oxidase
in the respiratory chain, completely stopping the absorption of oxygen by tissues and leading to death. If liver function is impaired, the risk of poisoning increases. The rate of sodium nitroprusside infusion should not exceed the body's ability to eliminate cyanide and should not last longer than 24 hours.
- In case of low blood pressure, the use of nitroprusside is contraindicated.
- Pregnant women should also not take it, since nitroprusside penetrates the placenta.
- For dissecting aortic aneurysm, sodium nitroprusside should only be used in combination with intravenous beta blockers because the drug increases the rate of blood ejection from the ventricles, which may promote the spread of the aneurysm.
Side effects
sodium nitroprusside:
- stomach pain, nausea, vomiting,
- severe hypotension,
- nephrotoxicity (kidney toxicity),
- tachycardia, shortness of breath,
- headache, dizziness, loss of consciousness,
- nervousness,
- vitamin B12 deficiency ( cyanocobalamin
).
With a high rate of administration of sodium nitroprusside, manifestations of cyanide or thiocyanide poisoning may develop with a clinical picture of coma
:
- pink skin color,
- weak pulse and breathing,
- pupil dilation.
With prolonged infusion and in cases of impaired renal function, it is necessary to monitor the level of thiocyanides
in blood plasma.
Pink skin color
(does not change even in a corpse) in combination with severe shortness of breath occurs in 2 cases: with
cyanide poisoning (hydrocyanic acid)
and with
carbon monoxide
(CO) poisoning.
However, the presence of a bitter almond odor
excludes CO poisoning (i.e., cyanide poisoning will result in pink skin color and a bitter almond odor).
Bitter almonds contain the glycoside amygdalin
, which (under the influence of the emulsin enzyme) easily decomposes into sugar, benzaldehyde and hydrocyanic acid. Therefore, bitter almond seeds, which contain up to 3.5% amygdalin, should not be eaten.
To be continued…
Same medicines, but different diseases
Patients are most aware of tablets prescribed for hypertension, osteochondrosis, or vasodilators, which are very useful for the brain and lower extremities, in general, about those medications that treat the most common diseases of our time.
For the brain
For example, for the brain, or rather, for improving its blood supply and nutrition, but depending on the nature of the cerebrovascular accident, representatives of different pharmacological groups are often suitable:
- Calcium antagonists that prevent Ca++ from entering the cell (cinnarizine, nimodipine);
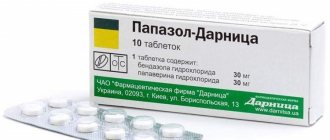
- Myotropic antispasmodics, relaxing the smooth muscles of blood vessels (no-spa, papaverine);
- Ergot alkaloids (due to their alpha-adrenergic blocking ability: dihydroergotoxin, vasobral);
- Drugs that correct cerebral circulation, which are called vascular drugs (Cavinton, Complamin, Trental, nicotinic acid);
- Vasodilators that block adrenergic receptors (adrenergic blockers: atenolol, timolol, propranolol, metoprolol);
- Other drugs that have the ability to act on blood vessels and increase their lumen, thereby improving cerebral circulation (vincamine, chimes, magnesium sulfate, dibazole).
For hypertension
The use of vasodilator drugs for hypertension, as a rule, implies their use for the brain, which, in conditions of vasoconstriction due to arterial hypertension, experiences serious suffering, not receiving nutrients carried by the blood. First of all, these are slow calcium channel blockers and adrenergic blockers.
Meanwhile, the list of drugs prescribed for hypertension is so large that it is simply impossible to list all the representatives. There are times when blood pressure requires immediate and rapid reduction. Of course, medications such as, say, benzohexonium (a ganglion blocker), which can be used in such cases, cannot be prescribed independently. Most of these medications are quite serious and require individual selection and the mandatory participation of a doctor. Examples include:
- Drugs that have a depressing effect on the vasomotor center (clonidine, dopegit);
- Substances that can block the transmission of nerve impulses in the ganglia of the ANS (ganglion blockers): benzohexonium, pentamine, pyrylene;
On the contrary, an attempt to quickly cope with a crisis using, for example, amlodipine (a slow calcium channel blocker) will also not lead to success.
But still, doctors more often have to deal with hypertensive patients, who must take medications that maintain blood pressure at a certain level. As a rule, such drugs are available in tablets or capsules and do not cause trouble to patients. People take them for years, gradually increasing the dosage of “their” medicine, or, on recommendation (and after selection), switch to other groups of vasodilators if the usual pills stop working or cause some kind of side effect.
Thus, in case of hypertension, to maintain blood pressure within normal limits, the following groups of medications are most often prescribed, which, however, are also selected on an individual basis, but are mainly available in pharmacies without a prescription:
- Adrenergic blockers (alpha and beta blockers);
- Slow calcium channel blockers;
- Angiotensin-converting enzyme inhibitors (ACE inhibitors);
- Angiotensin II antagonists;
- Renin inhibitors.
Lists of drugs - the main representatives of the above groups are not given in this section, since a more detailed description of these vasodilators will follow below.
For osteochondrosis
People who are faced with such a problem as cervical osteochondrosis can probably tell that due to such a disease, the vessels of the head are constantly in uncomfortable conditions. All this changes blood pressure, affects the state of memory and attention (the head becomes “heavy” and “difficult to think”), as well as general well-being (pain, discomfort, sleep disturbance, decreased ability to work). The use of vasodilators and damage to other parts of the spine cannot be ruled out. Thus, for osteochondrosis, in addition to anti-inflammatory drugs (NSAIDs), muscle relaxants such as mydocalm, agents that optimize the course of metabolic processes in tissues (mildronate, riboxin) and B vitamins, vasodilators are also used (xanthinol nicotinate, no-spa, papaverine), whose role is to improve blood supply to tissues.
For lower limbs
Vasodilator drugs are also used for diseases of the blood vessels of the arms and legs. However, impaired tissue nutrition as a result of narrowing of blood vessels is more typical for the lower extremities, therefore, the treatment of such pathological conditions is addressed more often and vasodilators, including peripheral vasodilators, are used mainly for the lower extremities (mainly for obliterating endarteritis, atherosclerosis, diabetic angiopathy):
- Myotropic antispasmodics (papaverine, no-shpa, drotaverine);
- Drugs with an adenosine mechanism of action (curantil, parsedil);
- Ergot alkaloids (vasobral, sermion);
- Leukotrienes and prostaglandins (Ventavis, Vazaprostan);
- Purine derivatives (agapurine, trental, pentoxifylline);
- Ganglion-blocking drugs (pentamine, dimecoline, benzohexonium);
- Calcium antagonists (felodipine, nifedipine, octidipine);
- Adrenergic blockers (phentolamine);
- Angiotensin-converting enzyme inhibitors (enalapril, lisinopril, ramipril).
The list of drugs could be continued indefinitely, meanwhile, the reader probably noticed that many groups and names of representatives have already been found in lists recommended for the treatment of other diseases.
Newspaper "News of Medicine and Pharmacy" 19 (436) 2012
Chronic heart failure (CHF) is a serious medical, social and financial problem. CHF affects almost 1.5–2% of the entire world population, and the incidence is 5–10 cases per 1000 people annually. The prevalence of CHF in the European population reaches 2.0%, in the USA - 2.2%, in Russia - 6% and increases significantly with age. According to the Rotterdam study, the prevalence of CHF among people aged 55-64 years is 1%, among people aged 75-84 years - 7%, and among people over 85 years old - more than 10%. 2–3% of all funds allocated for healthcare needs are spent on providing medical care to patients with chronic heart failure. At the same time, 70–80% of all financial costs for CHF fall on payment for inpatient treatment of the patient due to decompensation of the disease.
Chronic heart failure is a syndrome that develops as a result of various diseases of the cardiovascular system, leading to a decrease in the pumping function of the heart, chronic hyperactivation of neurohormonal systems, and manifested by shortness of breath, palpitations, increased fatigue, limited physical activity and excessive fluid retention in the body.
It should be noted that general practitioners need to remember that the severity of symptoms of CHF can be completely different - from minimal manifestations that occur only when performing significant loads, to severe shortness of breath that does not leave the patient even at rest. CHF is a progressive syndrome, and those patients who today have only hidden symptoms, within 1–5 years can become the group of the most severe patients who are difficult to treat. Therefore, early diagnosis of CHF, and therefore early initiation of treatment for such patients, is the key to success in the treatment of heart failure.
CHF syndrome can complicate the course of almost all diseases of the cardiovascular system. But the main causes, accounting for more than half of all cases, are coronary heart disease (CHD), arterial hypertension, or a combination of these diseases. In IHD, the development of acute myocardial infarction with subsequent focal decrease in myocardial contractility and dilation of the left ventricular cavity (remodeling) is the most common cause of CHF. With long-term chronic coronary insufficiency without myocardial infarction, loss of myocardial viability, diffuse decrease in contractility, dilatation of the heart chambers and the development of symptoms of CHF may progress. This situation is interpreted in the world as ischemic cardiomyopathy. In arterial hypertension, changes in the myocardium of the left ventricle, called “hypertensive heart,” can also cause CHF. Moreover, in many such patients, myocardial contractility and left ventricular ejection fraction (LVEF) remain normal for a long time, and the cause of decompensation may be disturbances in the diastolic filling of the heart with blood. The cause of the formation of right ventricular heart failure, as a rule, is chronic pulmonary heart disease, which develops as a result of pulmonary arterial hypertension caused by pathology of the bronchopulmonary apparatus, pulmonary vessels or thoracodiaphragmatic disorders. This disease ranks third among the causes of cardiovascular death, after myocardial infarction and arterial hypertension, and the two-year survival rate of patients with a detailed clinical picture is no more than 45%.
The main trigger of chronic heart failure is a decrease in myocardial contractility and, as a result, cardiac output. This, in turn, leads to a deterioration in the blood supply to organs and tissues and the activation of a number of compensatory mechanisms, one of which is hyperactivation of the sympathoadrenal system (SAS). Catecholamines, mainly norepinephrine, cause constriction of arterioles and venules, which causes an increase in venous return of blood to the heart, an increase in diastolic filling of the affected left ventricle and a leveling of reduced cardiac output to normal. However, activation of the SAS, being initially compensatory, subsequently becomes one of the factors responsible for the progression of pathological changes in the organs of the cardiovascular system and the aggravation of signs of heart failure. Spasm of arterioles, in particular renal arterioles, causes activation of the reninangiotensin system (RAS) and overproduction of a powerful vasopressor factor, angiotensin II. In addition to increasing the content of angiotensin II in the blood plasma, local tissue RAS are activated, in particular in the myocardium, which causes the progression of its hypertrophy. Angiotensin II also stimulates increased formation of aldosterone, which in turn increases sodium reabsorption, increases plasma osmolarity and, ultimately, promotes the activation of the production of antidiuretic hormone (ADH) - vasopressin. An increase in the content of ADH and aldosterone leads to a progressive retention of sodium and water in the body, an increase in the mass of circulating blood, and an increase in venous pressure. There is a further increase in venous return of blood to the heart, resulting in worsening left ventricular dilatation. Angiotensin II and aldosterone, acting locally in the myocardium, lead to changes in the affected part of the heart - so-called remodeling. In the myocardium, further death of myocardiocytes occurs and fibrosis develops, which further reduces the pumping function of the heart. Reduced cardiac output leads to an increase in residual systolic volume and an increase in end-diastolic pressure in the left ventricular cavity. Dilatation increases even more. This phenomenon initially, according to the Frank-Starling mechanism, leads to increased contractile function of the myocardium and equalization of cardiac output. However, as dilatation progresses, the Frank-Starling mechanism stops working, and therefore the pressure in the overlying parts of the bloodstream - the vessels of the pulmonary circulation - increases.
Among the neurohormonal disorders in CHF, one should note an increase in the content of endothelin in the blood, a powerful vasoconstrictor factor secreted by the endothelium.
Along with vasopressor factors, the content of atrial natriuretic peptide (ANP), secreted by the heart into the bloodstream, increases, which is associated with an increase in the tension of the atrial walls, with an increase in the filling pressure of the corresponding chambers of the heart. ANP dilates the arteries and promotes the excretion of salt and water. However, in CHF, the magnitude of this vasodilatory effect of angiotensin II and catecholamines and the potentially beneficial effects of APN on renal function are weakened. Thus, in the pathogenesis of CHF, cardiac and extracardiac mechanisms are distinguished. In this case, the triggering factor is the cardiac mechanism - a decrease in the contractile function of the heart or impaired filling of the heart during diastole.
The main link in the pathogenesis of chronic pulmonary heart disease is a decrease in the total cross-section of the pulmonary vessels due to spasm of the small pulmonary arteries in response to alveolar hypoxia. This leads to an increase in total pulmonary vascular resistance and pressure in the pulmonary circulation. Under these conditions, the right sections of the heart, and primarily the right ventricle, experience pressure overload, and later, with the development of tricuspid valve insufficiency, volume overload. As a consequence, hypertrophy and dilatation of the right chambers of the heart occurs. As the disease progresses, compensation may fail—right ventricular heart failure develops, which is the terminal stage of this condition.
Currently, the following classification of circulatory failure is used, proposed by N.D. Strazhesko:
- Stage I (initial) is characterized by latent circulatory failure, which is manifested by shortness of breath, palpitations and fatigue only during physical exertion. With rest, these phenomena disappear. Hemodynamics at rest are not impaired;
- Stage II, period A: signs of circulatory failure at rest are moderate, exercise tolerance is reduced. There are hemodynamic disturbances in the systemic or pulmonary circulation, their severity is moderate;
- period B: pronounced signs of heart failure at rest, severe hemodynamic disturbances in both the systemic and pulmonary circulation;
- Stage III (final) is characterized by dystrophic changes with pronounced hemodynamic disturbances, metabolic disorders and irreversible changes in the structure of organs and tissues.
The clinical picture of CHF is characterized by the following symptoms:
1. Dyspnea is the most common symptom of CHF and is inspiratory in nature. At the beginning, it appears only during physical activity, then it becomes constant, even at rest, turning into orthopnea - a high degree of shortness of breath with the patient in a forced position. Occurs in 98.4% of patients with CHF.
2. There may be attacks of cardiac asthma - acute suffocation in a “heart” patient.
3. A cough often accompanies shortness of breath in patients with chronic left ventricular failure, especially at night: dry, unproductive, with the discharge of mucous sputum.
4. Fatigue is the second symptom of heart failure after shortness of breath (in terms of sensitivity). Detected in 94.3% of patients suffering from CHF.
5. Palpitations are the third most frequently detected symptom of CHF (80.4%), which is expressed in the patient feeling each contraction of his heart. It is most often felt with tachycardia, but can be with a normal heart rate and even bradycardia.
6. Edema detected by patients with CHF indicates that the volume of extracellular fluid is increased by more than 5 liters. There is a pronounced dependence of edema on the position of the body: it spreads from bottom to top. Edema is traditionally associated with right ventricular failure, but it can also occur with decreased contractility of the left ventricle. Edema, caused predominantly by right ventricular failure and venous stagnation, usually appears later than the liver enlarges, they are extensive, dense to the touch, the skin under them is changed, cyanotic, with trophic changes. Edema with left ventricular dysfunction occurs earlier than venous stasis, is small, soft, removable, located in areas of the body remote from the heart, the skin underneath is pale.
7. A feeling of heaviness or pain in the right hypochondrium in patients with right ventricular failure usually precedes the appearance of edema, since the liver is the first to respond to failure of the right half of the heart. With the progression of CHF and prolonged stagnation, symptoms of liver dysfunction appear - icterus of the skin and mucous membranes, and portal hypertension occurs.
8. Nausea, vomiting, loss of appetite, constipation, flatulence and other symptoms of gastric and intestinal dyspepsia are almost constant companions of congestive heart failure.
9. A decrease in diuresis is associated with a significant decrease in renal blood flow, a reflex spasm of the renal arterioles and an increase in pressure in the renal veins. Urine is excreted mainly at night, due to some improvement in the blood supply to the kidneys at rest.
10. Complaints about decreased mental performance and mood, irritability, insomnia at night, drowsiness during the day.
Objective signs of cardiac dysfunction include data from mandatory instrumental and laboratory studies. Electrocardiography (ECG) is the most accessible instrumental method that allows you to objectively assess the condition of the heart. When analyzing the ECG, you should pay attention to the presence of signs of hypertrophy of the right and left parts of the heart, ischemic and cicatricial changes in the myocardium, the occurrence of disturbances in the conduction system of the heart and the presence of arrhythmias. A chest x-ray is necessary. In this case, when suspected of CHF, the main attention should be paid to cardiomegaly and venous pulmonary stasis. Cardiomegaly is evidence of the involvement of the heart in the pathological process. The presence of venous stagnation and its dynamics can be used to characterize the severity of the disease and serve as an objective criterion for therapy. In laboratory tests, a general blood test reveals compensatory erythrocytosis with an increase in hemoglobin levels. When determining hematocrit, an increase in hemoconcentration is often determined. Electrolyte blood tests, serum creatinine and glomerular filtration rate, blood glucose, liver enzymes, and urinalysis are also performed. Natriuretic hormones are used as markers in the diagnosis of heart failure, as well as to monitor the effectiveness of treatment. Echocardiography allows you to solve the main diagnostic problem - to clarify the very fact of dysfunction and its nature, to conduct a dynamic assessment of the state of the heart and hemodynamics.
According to the recommendations of the European Society of Cardiology (2008), ACE inhibitors, beta-adrenergic receptor blockers, angiotensin II receptor antagonists, aldosterone antagonists and peripheral vasodilators should be used in the treatment of patients with chronic heart failure. However, when choosing therapy, it is necessary to take into account the fact that most patients suffering from CHF are elderly, which means that adverse reactions when taking medications occur much more often and are more severe. In elderly patients, it is much more difficult to control the effectiveness of therapy due to multimorbidity, and they also have significantly lower adherence to therapy.
According to the EuroHeart Failure Survey registry (Komajda M. et al., 2003), in patients with heart failure, vasodilators are used in more than 30% of cases, that is, almost as often as beta-blockers and cardiac glycosides. However, the need for their additional use increases in proportion to the functional class of heart failure. Moreover, according to the Acute Decompensated Heart Failure study, early (within the first 6 hours after hospitalization) intravenous use of vasodilators in patients with acute decompensated heart failure can significantly reduce the likelihood of death within 48 hours of treatment compared with late (after 6 hours). hospital period) by their purpose (Okraince K. et al., 2006).
Peripheral vasodilators have beneficial hemodynamic effects in heart failure: due to the venodilating effect, they reduce afterload on the heart, increase stroke volume, and reduce the degree of primary or secondary dilatation. But it must be remembered that nitrates in geriatric patients often cause headache, nausea, and decreased blood pressure with reflex tachycardia. In such patients, tolerance to nitrates occurs quite quickly, within a few weeks, when their effectiveness decreases and does not increase even with an increase in single and daily doses. In this regard, sydnonimine derivatives are considered as an alternative, the most studied representative of which is molsidomine (Sidnopharm). This drug has a unique ability to realize vasodilating potential due to the reversal of endothelial dysfunction at virtually any initial level of NO, as well as with high activity of suppressants of its synthesis.
The main mechanism of the antianginal effect of molsidomine (Sidnopharm) is to reduce preload on the heart and have a beneficial effect on myocardial metabolism, as a result of which its oxygen demand is sharply reduced. Molsidomine (Sidnopharm) reduces venous pressure, end-diastolic pressure in the ventricles and pressure in the pulmonary artery, dilates large coronary arteries, and also improves collateral circulation in atherosclerosis of the coronary vessels.
After oral administration, molsidomine (Sidnopharm) is metabolized in the liver, turning into a pharmacologically active derivative of SIN1, from which the unstable compound SIN1A is formed non-enzymatically, containing a free pharmacologically active NO group and decomposing in the blood and tissues to the pharmacologically inactive SIN1C. The spontaneous elimination of NO during these transformations, similar to the action of nitrates, consistently leads to relaxation of vascular smooth muscles and vasodilation (Kmill M., Ochmanski W., 1998).
At the same time, the molecular mechanism of the vasodilating effect of sydnonimines has an important difference from the corresponding mechanism of action of nitrates: the absence of preliminary interaction with SH groups to activate cGMP. Due to this feature of molsidomine (Sidnopharm), clinically significant tolerance to it does not develop.
In patients with angiographic confirmation of coronary artery disease and heart failure, during long-term (for 4 weeks) therapy with molsidomine (Sidnopharm) at a dose of 4 mg 3 times a day per os, with increased performance and better exercise tolerance, the development of tolerance was not detected (Jansen W. et al., 1987).
SIN1 retains vasodilating activity even in patients with proven tolerance to organic nitrates, which is a reflection of the protective effect of the drug on the vascular endothelium. Its intravenous or intracoronary administration has a rapid vasodilating effect, not accompanied by steal syndrome (Berezin A.E., 2010). The results of repeated coronary angiography in several projections before and 2 minutes after intracoronary injection of SIN1 at a dose of 1 mg, as well as before and after the second injection 60 minutes later, showed an increase in the average diameter of 44 normal segments of the left coronary artery by 12% immediately after the injection of SIN1 and by 8 % - after 60 minutes (Serruys PW et al., 1987).
In a randomized, double-blind, placebo-controlled study, the use of molsidomine (Sidnopharm) in patients with coronary artery disease at a dose of 12 mg/day for 48 hours increased flow-mediated vascular dilatation by 60% after the first dose of the drug (Herman AG, Moncada S., 2005).
The antiplatelet properties of molsidomine (Sidnopharm) and its active metabolite SIN1 were studied when administered orally in healthy volunteers and intravenously in patients with myocardial infarction (Wautier JL et al., 1989), as well as in comparison with similar properties of isosorbide 5 mononitrate and placebo. In contrast to isosorbide 5 mononitrate, 30 and 60 minutes after the use of molsidomine (Sidnopharm) there was a significant (100 and 120%, respectively) increase in threshold levels of platelet activating factor, which caused their irreversible aggregation, and a significant decrease in aggregation curves, which is very important in the treatment of heart failure .
A number of specially designed randomized controlled studies revealed a favorable hemodynamic and clinical effect of molsidomine (Sidnopharm) in patients with heart failure resulting from coronary artery disease, arterial hypertension, cardiomyopathy and chronic obstructive pulmonary disease (Kmiec M., Ochmanski W., 1998). W. Rudolph, J. Sirshinger (1985) noted not only an increase in left ventricular ejection fraction, but also a significant regression of clinical symptoms of the disease, increased tolerance to physical activity, and improved quality of life with a completely acceptable tolerability profile of this drug.
In patients with reduced left ventricular EF, the addition of molsidomine (Sidnopharm) at a dose of 6 mg/day to standard therapy was accompanied by a significant significant increase in LVEF after 3 months of its use (Spring A. et al., 1998). According to N.M. Mukharlyamov and V.Yu. Mareeva (1985), during treatment with molsidomine (Sidnopharm) in single doses of 6–8 mg, pronounced clinical and hemodynamic (objectified by the results of echocardiography and pulmonary artery catheterization) improvement was observed in patients with severe decompensated chronic heart failure.
The clinical efficacy of adjuvant molsidomine (Sidnopharm) was assessed in patients with pulmonary hypertension. The trial recruited patients with heart failure secondary to documented pulmonary arterial hypertension who responded to inhaled synthetic prostaglandin or sildenafil at recommended doses. It turned out that a 24-hour intravenous infusion of molsidomine (Sidnopharm) is more effective in reversing signs of heart failure and the level of systolic pressure in the pulmonary artery than isosorbide 5 mononitrate (Lehmann G. et al., 1998).
Thus, Sidnopharm (molsidomine) retains its position as a drug that can effectively control the symptoms of heart failure during combination therapy. Improvement in physical condition during therapy with Sydnopharm (molsidomine) allows patients to maintain not only daily, but also, in many cases, professional activity, if it is not associated with heavy physical labor, and the positive dynamics of physical and psychological status contributes to a significant improvement in the quality of life.
Prepared by T. Chistik
Points of application for vasodilators
Vasodilator drugs are a rather heterogeneous group, but, solving one problem (dilation of blood vessels), each drug goes its own way to achieve its goal. This means that for each subgroup of these medicinal substances there are their own points of application, while they remain “indifferent” to the rest, for example:
- Some are busy blocking alpha and beta adrenergic receptors;
- Others are responsible for regulating the activity of the RAAS (renin-angiotensin-aldosterone system);
- Still others generally refer to calcium antagonists, which block slow calcium channels and thereby prevent the flow of this chemical element into the cell so that its concentration does not reach life-threatening digital values;
- Fourth, they directly relax smooth muscles, affecting the cells of smooth muscle fibers (this refers to myotropic antispasmodics, for example, no-spa, papaverine, which are used not so much to lower blood pressure, but to alleviate the symptoms of other diseases).
Vasodilators are widely used in medical practice in the treatment of various pathological conditions:
- For hypertension;
- Coronary heart disease;
- Chronic heart failure:
- Diseases caused by impaired peripheral circulation;
- Diseases of the brain associated with a decrease in the lumen of cerebral vessels as a result of their narrowing;
- Diabetes mellitus and complications of this pathology;
- Vegetative-vascular dystonia;
- Arthrosis;
- Diseases of the organs of vision.
In this regard, it would probably be appropriate to somewhat explain to the reader the essence of the mechanisms listed above, because most patients, knowing that their vessels are narrowed and need to be dilated, correctly name the groups of drugs (for example, β-blockers, calcium antagonists, etc. .), but at the same time have no idea what this or that drug does in their body and how a positive result is achieved or the treatment does not give the expected effect if the drug is chosen incorrectly. The following sections may be of interest to patients who wish to understand in more detail the mechanisms of action of vasodilators.
Mechanisms of action of vasodilators
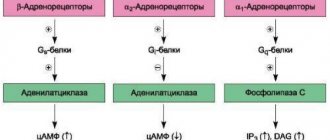
Blockade of α- and β-adrenergic receptors
Excessive exposure to various biologically active substances (biologically active substances), in particular adrenaline, causes a decrease in the lumen of blood vessels, which is manifested primarily by an increase in blood pressure. In order to neutralize the negative (vasoconstrictor) effect of these substances, the patient is prescribed medications that have the ability to block adrenergic impulses and, thus, neutralize the effects of biologically active substances.
Adrenergic blockers represent a fairly broad group of drugs, which, however, depending on the receptors that they can act on and block, is divided into 2 subgroups: α- and β-adrenergic receptor blockers. The first list of drugs (α-blockers) includes:
- Terazosin;
- Silodosin;
- Alfuzosin;
- Yohimbine;
- Nicerogolin;
- Dihydroergotoxin;
- Phentolamine;
- Proroksan.
The second list of drugs that block adrenergic receptors (beta) can be represented by drugs that are easily recognized by the ending “-olol”:
- Atenolol:
- Metoprolol;
- Bisoprolol;
- Esmolol;
- Oxprenolol;
- Metypranolol;
- Propranolol.
In addition, in the group of β-blockers, cardioselective (atenolol, metoprolol, esmolol) and non-selective beta 1,2-adrenergic blockers (sotalol, propranolol, timolol) are distinguished; the group of alpha blockers is also divided into several subgroups: α-1, α- 2, α-1,2-adrenergic blockers.
Inhibition of angiotensin-converting enzyme
The functioning of the RAAS is disrupted as a result of many pathological processes triggered by stimulation of renin production in the kidneys, disruption of the production of the hormone aldosterone in the adrenal glands, and synthesis of the glycoprotein agiotensinogen in the liver.
Renin entering the blood reacts with angiotensinogen, converting it into angiotensin I, which, in turn, under the influence of the ACE enzyme is transformed into angiotensin II, a powerful vasoconstrictor component. Angiotensin II, in addition, provokes a spasm of smooth muscle fibers and, by its presence, disrupts the adequate synthesis of bradykinin, while simultaneously promoting the stimulation of aldosterone production, and this leads to a decrease in the internal diameter of blood vessels, an increase in blood pressure, and impaired blood circulation in the microvasculature.
Obviously, to prevent the development of such a reaction and the formation of angiotensin II as a result, it is necessary to suppress the synthesis of the ACE enzyme. This role has been assigned to vasodilator drugs called angiotensin-converting enzyme inhibitors or ACE inhibitors (ACEIs). This is an accessible, very popular, and widespread group. Most often, ACE inhibitors are used for hypertension and other pathological conditions of the cardiovascular system.
an example of the effect of ACE inhibitors in chronic heart failure
The list of ACE inhibitor drugs is quite wide, where patients suffering from arterial hypertension are very familiar with drugs that, like beta blockers, also have their own distinctive particle at the end of the word (“-adj”):
- Captopril;
- Enalapriril;
- Lisinopril;
- Monopril;
- Ramipril;
- Accupril;
- Quinapril.
Individual angiotensin-converting enzyme inhibitors for hypertension are prescribed immediately in the form of combined drugs (with diuretics - enam N, lysiton N, capozide or calcium antagonists - equator).
Blockade of individual (slow) calcium channels
scheme of cardiomyocyte overload with calcium ions
It turns out that calcium, which is so vital for muscle fibers to function fully, may not always be useful. The active movement of ions of this chemical element from the intercellular space through calcium channels into the cell and its excessive concentration in the cells can overload tissues that respond with excessive tension. Thus, tissues consisting of smooth muscle fibers can be damaged, regardless of their location (skeletal muscles, atrioventricular pathways, cardiac muscle myofibrils, blood vessels).
Medications that interfere with the movement of the ionized form of this element help prevent the penetration of unnecessary amounts of calcium (Ca++) into cells. They simply block slow calcium channels located in smooth muscle cells, which prevents the accumulation of Ca++. These medications relax smooth muscles (including blood vessels) and thereby reduce blood pressure; in addition, representatives of the group of calcium antagonists (as these pharmaceuticals are called) regulate heart rhythm.
Obviously, such substances in such cases take on the role of vasodilators. Commonly prescribed calcium channel blockers include:
- Nifedipine;
- Felodipine;
- Lacidipine;
- Amlodipine;
- Verapamil;
- Diltiazem.
Most calcium antagonists can also be recognized by the ending of their names ("-dipin").
Figure: example of the action of calcium antagonists
NEWS LIBRARY LINKS ABOUT THE SITE
c) Myotropic vasodilators
Substances in this group act directly on the smooth muscle fibers of blood vessels, causing them to relax. As a result, the blood vessels dilate; dilation of arterial vessels leads to a decrease in blood pressure. Myotropic vasodilators inhibit the vasoconstrictor effects of both the sympathetic nervous system and the renin-angiotensin system.
Apressin
(hydralazine) dilates mainly arterial vessels and has little effect on the tone of the veins, therefore, orthostatic hypotension does not occur with its use.
A decrease in blood pressure when using apressin is accompanied by tachycardia and an increase in renin secretion. Therefore, it is advisable to combine the drug with substances that reduce the influence of the sympathetic nervous system (β-blockers, reserpine). Apressin is prescribed orally in tablets; duration of action is 6-12 hours. Side effects
: nausea, headache, dizziness, skin rashes; in large doses, the drug can cause systemic lupus erythematosus syndrome.
Diazoxide
(hyperstat) primarily dilates arterial vessels. When it enters the blood, it is almost completely bound by blood plasma proteins and in this state does not show activity. The drug is quite effective only when administered intravenously, since only in this case it is possible to create a sufficient concentration of the free drug, not bound to plasma proteins, in the blood. Diazoxide is one of the best drugs for relieving hypertensive crises. Duration of action 3-12 hours.
Sodium nitroprusside
- one of the most effective antihypertensive drugs with myotropic action: it dilates both arterial and venous vessels. Solutions of the drug are administered intravenously by drip (with a single injection, the duration of action of the drug is 2-5 minutes). Sodium nitroprusside is used to relieve hypertensive crises and for controlled hypotension.
Magnesium sulfate
reduces blood pressure only with parenteral (intramuscular, intravenous) administration. When administered orally, the hypotensive effect usually does not develop, since the drug is poorly absorbed from the gastrointestinal tract.
The mechanism of the hypotensive effect of magnesium sulfate is complex. Basically, the vasodilating effect of the drug is associated with its myotropic antispasmodic properties. In addition, the drug has a weak ganglion-blocking effect and the ability to inhibit the vasomotor center. The last property of magnesium sulfate is associated with its narcotic activity.
Magnesium sulfate is used most often during hypertensive crises and nephropathy (late toxicosis of pregnancy, accompanied by increased blood pressure) to quickly lower blood pressure.
As an antihypertensive agent, magnesium sulfate solutions are most often administered intramuscularly.
If intramuscular injections of magnesium sulfate are ineffective, they resort to intravenous administration, which, however, should be carried out with extreme caution. When administered intravenously, the narcotic properties of magnesium sulfate are especially clearly manifested, and since the narcotic breadth of the drug is small, in this case respiratory depression easily occurs.
At the first signs of respiratory depression, administration of the drug should be stopped and an antagonist of magnesium sulfate - calcium chloride or calcium gluconate - should be administered intravenously.
Dibazol
used most often for the treatment of hypertensive crises. In these cases, the drug is administered intravenously. When administered orally, dibazole is ineffective.
New on atreya-ayurveda.ru Ayurvedic clinic on Osennyaya street, building 16
High popularity of vasodilators among the people
The high popularity of vasodilator drugs is explained by their widespread use in many pathological conditions, however, not all patients are in a hurry to take drugs obtained synthetically, because drugs that can dilate blood vessels and improve blood supply can be extracted from natural sources.
Substances that can have a positive effect on human blood vessels are carried by many representatives of the plant world. Some of them become the basis for obtaining medicines sold by pharmacy chains (for example, ginkgo biloba), others can be collected independently and prepared as a medicinal product at home. From plants such as Baikal skullcap, hawthorn (flowers and berries), parsley (seeds), basil, oregano, knowledgeable people prepare infusions, decoctions, and squeeze out oils. But this may be an auxiliary treatment or assistance in the first stages of the disease.
Video: review of folk vasodilators
In other cases, you will have to resort to medications produced by the pharmaceutical industry, and here I would like to warn patients: only a doctor knows which synthetic vasodilator drugs will help a person endure the course of chronic processes relatively painlessly, that is, self-medication will be inappropriate.